Introduction
Lice have been associated with humans throughout written history. In fact, human-infesting lice get their common names from the areas of the human body where they are typically found. Outbreaks often occur in crowded and/or unsanitary conditions when people cannot bathe or wash their clothing regularly. However, lice may become a problem in sanitary environments as well. As with pests such as bed bugs, human lice transcend socio-economic boundaries. Nonetheless, unfortunately, people with limited financial resources often lack the ability to cope with severe problems. Each year in North Carolina, county health departments diagnose several hundred cases of human lice ("pediculosis"), primarily head lice. This estimate probably represents only the "tip of the iceberg," since many cases likely go unreported because people consult their private physician for treatment. Human-infesting lice are considered both a medical and insect pest problem.
Biology and Life Cycle
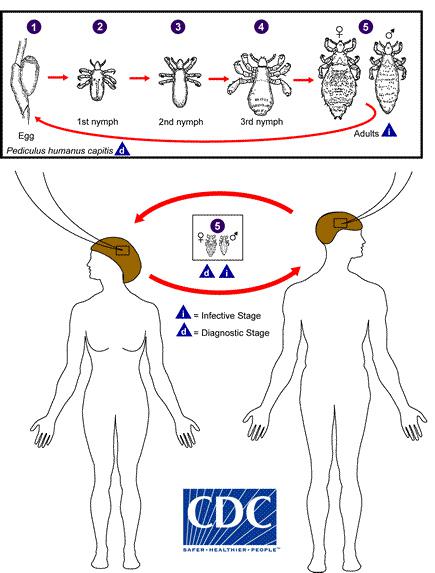
Lice as a group are small, wingless insects with flattened, elongate bodies and somewhat oval heads. There are slight differences in morphology that distinguish head, pubic, and body lice from one another, but these features are difficult to observe without a microscope. Although small, lice are visible to the naked eye and range in size from 1/16 to 1/8th of an inch in length. They are dirty white to grayish black in color. Lice are wingless. They do not jump (like fleas) or fly (like mosquitoes). Lice live continuously on the host and have a three stage life cycle (egg, nymph and adult), as shown below. The nymphs molt three times before reaching maturity. Newly hatched nymphs (first instars) must take a blood meal quickly after emergence, or they can die. Adults typically live for 20-30 days depending on the species. Below, we will focus on more detailed characteristics of head lice (Pediculus humanus capitatus), body lice (Pediculus humanus humanus) and pubic lice (Pthirus pubis).
Head Lice
Head lice (Pediculus humanus capitatus) (Figure 1) live on the scalp and, for all practical purposes, occur only on the head. Adult female lice glue eggs ("nits") to the base of a hair shaft, frequently behind the ears or on the nape of the neck. Nits require high heat and humidity to develop. If conditions are supportive, nits will hatch in about 5-10 days and the light-colored nymphs begin feeding immediately. If the first instar does not feed within 24 hours post-emergence, it will die. Development from egg to adult takes approximately 3 weeks. The adult life stage can survive for 20 or so days in ideal conditions. Head lice will infest clothing and other items that come in contact with the head (e.g., hats, shirt collars, barrettes, brushes, combs, etc.), but they do not survive off of a person for more than about 48 hours.
Head lice are not known to transmit any disease organisms. However, their feeding activity irritates the scalp, causing intense itching. Secondary infections can result if the skin is broken by repeatedly scratching affected areas of the scalp. The most notable impact of head lice is the personal embarrassment experienced with being identified publicly as having lice (e.g., in a classroom). Children, particularly those of elementary and middle school age, are most likely to get head lice because of their close contact and social interactions with each other. Close contact at school, daycare, etc., creates opportunities for the lice to be spread among children very easily. Children who become infested in school will carry lice home and may infest family members who then become a source for recurring louse problems within the home.
Managing Head Lice
Remedying a head lice infestation is difficult if cooperation from all affected individuals is not achieved. Parents should notify the school principal or nurse immediately if their child has a confirmed case of head lice. Do not be embarrassed by the problem and hesitate to call personnel at school, daycare, or anywhere else that the child spends copious amounts of time. It is important to remember that, firstly, just because your child has head lice does not necessarily mean that he/she is the source of the problem. Second, and most importantly, if school officials do not take any action because they are unaware of the problem, lice will likely spread to other children in the class. If the problem continues unchecked, eventually even those children who were treated previously become reinfested and they must be subjected to treatment again.
Parents, school administrators, teachers and other school staff should handle these situations discretely, being sensitive to the children's situation which is difficult enough for them without the issue becoming a matter for public discussion. Children exhibiting symptoms of head lice (excessive head scratching and/or abrasions on the scalp) need to be checked for the presence of nits or live lice by someone who can positively identify the eggs or the insects. The whitish-to-cream colored eggs are small (about 1 mm) and oval with a distinct cap. To the unaided eye, nits can easily be confused with dandruff, globules of hair oil or even dried flakes of hairspray. For that reason, a "no-nit" policy can be unproductive because children may be kept out of school unnecessarily due to misidentification. Upon closer examination with a magnifying glass, the eggs are more easily recognized. On average, the actual number of head lice found on a person is low: about 5-10. Therefore, careful inspection of the head, particularly along the back of the neck and around the ears is important. Another useful way to check for lice is to have the person hold their head over a light-colored towel or piece of cardboard, then brush their hair and scalp vigorously towards the towel. Dislodged lice should be visible on the towel. Once a louse infestation is confirmed, you should take the appropriate control measures:
- Treat ALL infested persons. Check all family members, classmates and playmates. Anyone who is infested should receive proper treatment. There are several pediculicidal (lice-killing) shampoos/rinses that can be purchased at most drugstores. Many of the products contain pyrethrins; examples include RID®, A200®and R&C Shampoo®. Nix® contains permethrin which is similar in action to pyrethrins. Because of their extensive (and repeated) use, lice populations may be developing resistance to pyrethroid (and similar compounds) are there are some reports that over-the-counter products are failing. There are several prescription products with different 'modes of action' and may be necessary if other products have failed. These prescription products include "Ovide®" (which contains the insecticide malathion), "Sklice®" (an oral treatment containing ivermectin), and "Ulesfia®". These products work well against nymphs and adults, but some such as "Sklice" and "Ulesfia" are not effective against eggs. One or two additional treatments at 7-10 day intervals are sometimes needed in order to eliminate the infestation. entirely. Read and follow the instructions on the product labels carefully. Particularly when children are involved, we strongly recommend that you seek advice from your family physician or child's pediatrician about the best way to proceed in solving the problem quickly and safely. Because head lice spend so much time on the body versus the environment, they are considered a medical problem and should be treated as such. Pesticides applied in the environment do nearly nothing to reduce the presence of lice.
- Remove nits from hair. Mechanical removal of louse eggs helps reduce the number of lice that might hatch on the scalp. Since children who are declared "nit-free" by a doctor or school nurse can return to class sooner, removing nits has a positive impact on their morale and lessens disruption to their school and social activities. Special combs are provided with the pediculicides and the instructions for their use must be followed explicitly. Be persistent and thorough. Because the eggs are literally cemented to the hair shaft, they are not easily dislodged. Contrary to popular belief, using vinegar in a shampoo or as a rinse is not effective because it does not dissolve the glue that binds the nits to the hair shaft. There are also special non-insecticidal rinses, such as ClearTM Lice Egg Remover, that dissolve the glue binding the eggs to the hair. Nits are more easily removed after shampooing/rinsing, when the hair is still damp. Several combing sessions may be needed to remove all of the nits. More than one insecticidal treatment may be necessary, too.
- Delouse personal items. Although head lice cannot survive for long periods off of people, sanitation helps end the problem more quickly. Items such as brushes and combs should be washed thoroughly in hot water (at least 130o F) for 5-10 minutes. Washable clothing, hats, head bands, bed linen and other personal items should be washed in hot soapy water, then dried in a clothes drier for at least 20-30 minutes. Non-washable clothing can be dry-cleaned, but the expense is hard to justify when a simpler solution would be to isolate theses items for a few days. Vacuuming mattresses, upholstery, and carpeting will pick up stray lice. Although hair with attached lice eggs may fall out and become attached to stuffed animals or similar toys, such items do not serve as reservoirs for the lice. If there is some concern about these items carrying lice, the simplest solution is to vacuum them or (if possible) place them in a clothes dryer set on maximum heat for about 1 hour. Isolating items in a garbage bag for 5-7 days should also eliminate any active/hatching lice. Spraying furniture, carpeting and bedding with an insecticide serves no real purpose other than providing some margin of psychological comfort. Although such sprays kill an occasional stray louse, family members who are already being treated with insecticidal shampoos can be exposed unnecessarily to additional pesticides. We do not recommend spraying insecticides carpeting, furniture or other items.
The extent of delousing activities in a school depends largely on the age of the students and the layout of the classroom. As in the home, vacuuming carpeting and/or sleeping mats can help. Mats with vinyl or other non-fabric coverings can be cleaned with hot, soapy water. The same holds true for classroom desks and chairs. Clothing or personal items that students leave in closets, storage areas or desks should be removed and cleaned. Applying insecticides in the classroom is not necessary and it discouraged. School buses should not be a problem but the seats and headrests can always be cleaned with an appropriate cleaner. It is helpful if schools assign cubbies, wall hooks, lockers, and other areas with personal belongings to specific students. This prevents the cross-contamination of personal items.
Biology and Management of Body Lice
Body lice (Pediculus humanus humanus) look virtually identical to head lice, but their location on people is a reasonably accurate diagnostic clue. Head lice are found almost exclusively on the scalp, whereas body lice may be found either on the body or clothing. Unlike head lice, body lice attach their eggs to the fibers of undergarments, particularly along inside seams and other areas of close body contact. A female body louse usually deposits 9-10 eggs per day, for a total of 270-300 eggs over her lifetime. The eggs are incubated by the person's body heat and hatch in about one week. Temperatures above 100°F or below 75°F. reduce or completely stop egg hatch. Development time (egg to adult) is as short as 8-9 days if clothes stay in constant contact with the body. If clothing is removed nightly, development time may increase to 2-4 weeks.
Body lice are most common during the winter months, when people tend to wear layers of clothing, creating a warm, moist environment that is ideal for louse development. An important point to note is that body lice spend most of their life on clothing and crawl onto the host to feed for short periods. Although as many as 1,000 body lice have been removed from heavily infested clothing, ten lice per person is probably more typical. Body louse problems are more likely to occur in situations where the same clothing is worn constantly for several days or weeks. Since body lice can survive away from a person for 24-48 hours, they can survive in clothing that is removed nightly but worn again the following day.
Although body lice can transmit certain disease organisms, this problem is generally confined to underdeveloped countries where poor sanitation and overcrowding are major contributing factors. Feeding activity by the lice causes significant skin irritation, swelling and the formation of red welt-like marks. Severe infestations can lead to allergic reactions and skin disorders, such as impetigo and eczema. Treatment for body lice is virtually identical to the procedures for head lice. First, the infested person must be treated with pediculicides (lotions or shampoos). As in the case of head lice, body lice move rapidly from person to person upon brief contact or when clothing is shared. Other family members (or classmates) with whom the person comes in contact should be checked and treated, if necessary. Clothing, bed linen and other personal items that have been used recently must be deloused as outlined in Step #3 for head lice. Vacuuming mattresses, carpets and upholstery will help remove stray lice.
Biology and Management of Pubic Lice
Pubic or crab lice (Pthirus pubic) are usually found on the hairs in the pubic areas; however, they can be found among the coarser hairs of the chest, armpits, eyebrows, eyelashes, mustaches, and beards. Unlike body lice, crab lice are dark gray-to-brown in color. The name "crab lice" comes from their flattened, oval crab-like shape. Their second and third pairs of legs have thumb-like projections that aid in grasping the host's hair. Eggs of pubic lice are dark brown and smaller than those of head and body lice. The female lays about 30 eggs during her 3-4 week lifespan, usually on the hairs of the pubic region. Crab lice are more sedentary than body and head lice and usually pass their entire life cycle in the same area where the eggs were deposited.
Crab louse bites produce discrete, round slate-gray to bluish colored swellings on the skin. Proteins in the louse's saliva may cause an allergic reaction and intense itching. As with head lice, secondary bacterial infections may result from constant scratching and breaking the skin. Lice infesting the eyelids can cause severe inflammation and swelling around the eyes. Crab lice are not known to transmit disease organisms, but one survey found that one third of those with pubic lice simultaneousy suffered from a sexually-transmitted disease as well.
Crab lice are spread primarily through sexual and/or intimate contact. It is possible, but extremely rare, that they could be acquired through contact with infested toilet seats, clothing or bedding. As with other louse problems, successful treatment is based on a combination of sanitation and pediculicides. As with other louse problems, successful treatment is based on a combination of sanitation and pediculicides: Family members who share a bed with the infested person must be examined and treated if necessary. Undergarments and bed linens should be washed in hot water for at least 20 minutes, then dried on a high setting. Louse control products are available either directly at a drugstore or by prescription; however, we strongly recommend that infested persons first seek advice from their primary physician. Because crab lice can only survive off of a host for about 24 hours, insecticidal treatments in the home, workplace, school or other areas are neither necessary nor are they recommended.
Summary
Successful control of louse problems requires communication, cooperation, and a control program that employs sanitation, treatment with pediculicides and delousing of clothing and other personal articles. Solving the problem is more important than finding someone to blame for it. Open and frank discussion, quick action, and sensitivity to the embarrassment experienced by infested persons is needed by everyone involved.
For additional information, we recommend that you consult the National Pediculosis Association.
References used in preparing this publication:
Goddard, J. 1993. Physicians Guide to Arthropods of Medical Importance. CRC Press, Boca Raton, FL.
Smith, E.H. and R.C. Whitman. NPMA Field Guide to Structural Pests, Second Edition.
Publication date: May 1, 2003
Reviewed/Revised: Oct. 24, 2022
The use of brand names in this publication does not imply endorsement by NC State University or N.C. A&T State University of the products or services named nor discrimination against similar products or services not mentioned.
Recommendations for the use of agricultural chemicals are included in this publication as a convenience to the reader. The use of brand names and any mention or listing of commercial products or services in this publication does not imply endorsement by NC State University or N.C. A&T State University nor discrimination against similar products or services not mentioned. Individuals who use agricultural chemicals are responsible for ensuring that the intended use complies with current regulations and conforms to the product label. Be sure to obtain current information about usage regulations and examine a current product label before applying any chemical. For assistance, contact your local N.C. Cooperative Extension county center.
N.C. Cooperative Extension prohibits discrimination and harassment regardless of age, color, disability, family and marital status, gender identity, national origin, political beliefs, race, religion, sex (including pregnancy), sexual orientation and veteran status.